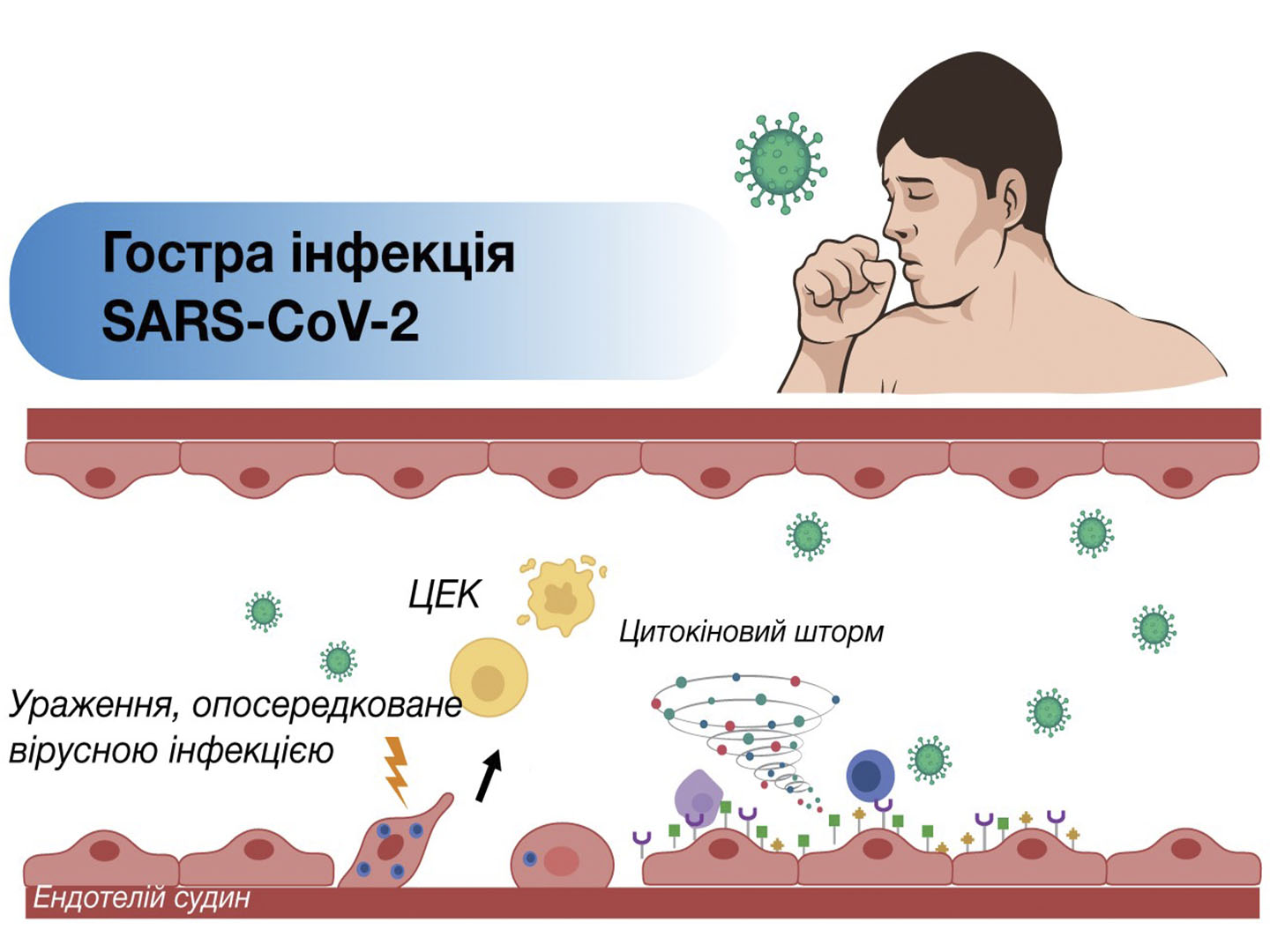
Cardioprotector effect of nitrogen oxide donor in patients with hypertension

Abstract. The last decade has been marked by the intensive development of basic and clinical research on the role of vascular endothelium in the genesis of cardiovascular disease (CVD).
Today, researchers are focused on studying the role of endothelial dysfunction (DE) in the pathogenesis of CVD, as well as to find ways to effectively correct it.
The article presents data from international and Ukrainian publications on the possible cardioprotective effect of nitric oxide donor in patients with hypertension.
Keywords: hypertension, cardioprotection, L-arginine.
Author: Tashchuk V.K., MD, Professor, Head of the Department of Internal Medicine, Physical Rehabilitation and Sports Medicine, Bukovynian State Medical University, Chernivtsi, Ukraine.
Literature:
- Марунич Р. Ю., Горницька О. В., Гудзенко А. В. та ін. (2021). Роль ендотелію в регуляції агрегатного стану крові в нормі при атеросклерозі та артеріальній гіпертензії. Фізіол. журн., Т. 67, № 3.
- Vane J. R., Anggård E. E., Botting R. M. (1990). Regulatory functions of the vascular endothelium. N Engl J Med. Jul 5; 323 (1): 27-36. doi: 10.1056/NEJM199007053230106.
- Smith O. (1998). Nobel Prize for NO research. Nat Med 4, 1215. https://doi.org/10.1038/3182.
- Furchgott R. F., Zawadzki J. V. (1980). The obligatory role of endothelial cells in the relaxation of arterial smooth muscle by acetylcholine. Nature. Nov 27; 288 (5789): 373-6. doi: 10.1038/288373a0.
- Palmer R.M., Ferrige A.G., Moncada S. (1987). Nitric oxide release accounts for the biological activity of endothelium – derived relaxing factor. Nature; 327: 524-6.
- Lim P. O., Young W. F., MacDonald T.M. (2001). A review of the medical treatment of primary aldosteronism. J Hypertens. Mar; 19 (3): 353-61. doi: 10.1097/00004872-200103000-00001.
- Canto J. G., Kiefe C. I., Rogers W. J. et al. (2011). Number of coronary heart disease risk factors and mortality in patients with first myocardial infarction. JAMA. Nov 16; 306 (19): 2120-7. doi: 10.1001/jama.2011.1654.
- Nilsson P. M. Early vascular aging (EVA): consequences and prevention. Vasc Health Risk Manag.; 4: 547-52. doi: doi.org/10.2147/VHRM.S1094.
- Schmitt M., Avolio A., Qasem A. et al. (2005). Basal NO locally modulates human iliac artery function in vivo. Hypertension. Jul; 46 (1): 227-31. doi: 10.1161/01.HYP.0000164581.39811.bd.
- Schillaci G., Verdecchia P., Porcellati C. et al. (2000). Continuous relation between left ventricular mass and cardiovascular risk in essential hypertension. Hypertension. Feb; 35 (2): 580-6. doi: 10.1161/01.hyp.35.2.580.
- Tomiyama H., Ishizu T., Kohro T. et al. (2018). Longitudinal association among endothelial function, arterial stiffness and subclinical organ damage in hypertension. Int J Cardiol. Feb 15; 253: 161-166. doi: 10.1016/j.ijcard.2017.11.022.
- Perticone F., Ceravolo R., Candigliota M. et al. (2001). Obesity and body fat distribution induce endothelial dysfunction by oxidative stress: protective effect of vitamin C. Diabetes. Jan; 50 (1): 159-65. doi: 10.2337/diabetes.50.1.159.
- Соколова Л. К., Пушкарьов В. М., Тронько М. Д. (2019). L-аргінін у нормі та патології. Ендокринологія. Vol. 24. № 4. 373-385. doi: 10.31793/1680-1466.2019.24-4.373.
- Weckman A. M., McDonald C.R., Baxter J. B. et al. (2019). Perspective: L-arginine and L-citrulline Supplementation in Pregnancy: A Potential Strategy to Improve Birth Outcomes in Low-Resource Settings. Adv Nutr. Sep 1; 10 (5): 765-777. doi: 10.1093/advances/nmz015.
- Quyyumi A. A., Dakak N., Diodati J. G. et al. (1997). Effect of l-arginine on human coronary endothelium-dependent and physiologic vasodilation. J. Am. Coll. Cardiol., 1997 – Vol. 30 – p. 1220-1227.
- Lerman A., Burnett J. C.J., Higano S. T. et al. (1998). Long-term l-arginine supplementation improves small-vessel coronary endothelial function in humans. Circulation, Vol. 97, p. 2123-2128.
- Міщенко Л. А. (2020). Органопротекторні можливості L-аргініну в лікуванні пацієнтів з артеріальною гіпертензією. «Здоров’я України 21 сторіччя» № 23 (492).
- Sepandi M., Abbaszadeh S., Qobady S. et al. (2019). Effect of L-Arginine supplementation on lipid profiles and inflammatory markers: A systematic review and meta-analysis of randomized controlled trials. Pharmacol Res. Oct; 148: 104407. doi: 10.1016/j.phrs.2019.104407.
- Yin W. H., Chen J. W., Tsai C. et al. (2005). L-arginine improves endothelial function and reduces LDL oxidation in patients with stable coronary artery disease. Clin Nutr. Dec; 24 (6): 988-97. doi: 10.1016/j.clnu.2005.07.003.
- Кутовой А. Б., Люлько И. В., Амро А. и др. (2014). L-Аргинин в комплексной терапии хронической ишемии нижних конечностей при атеросклерозе. Серце і судини, № 3, С. 89-92.
- Lekakis J. P., Papathanassiou S., Papaioannou T. G. et al. (2002). Oral L-arginine improves endothelial dysfunction in patients with essential hypertension. Int J Cardiol. Dec; 86 (2-3): 317-23. doi: 10.1016/s0167-5273(02)00413-8.
- West S. G., Likos-Krick A., Brown P. et al. (2005). Oral L-arginine improves hemodynamic responses to stress and reduces plasma homocysteine in hypercholesterolemic men. J Nutr. Feb; 135 (2): 212-7. doi: 10.1093/jn/135.2.212.
- Bahadoran Z., Mirmiran P., Tahmasebinejad Z. et al. (2016). Dietary L-arginine intake and the incidence of coronary heart disease: Tehran lipid and glucose study. Nutr Metab (Lond). Mar 15; 13: 23. doi: 10.1186/s12986-016-0084-z.